Healthcare Performance & Patient Safety Analytics
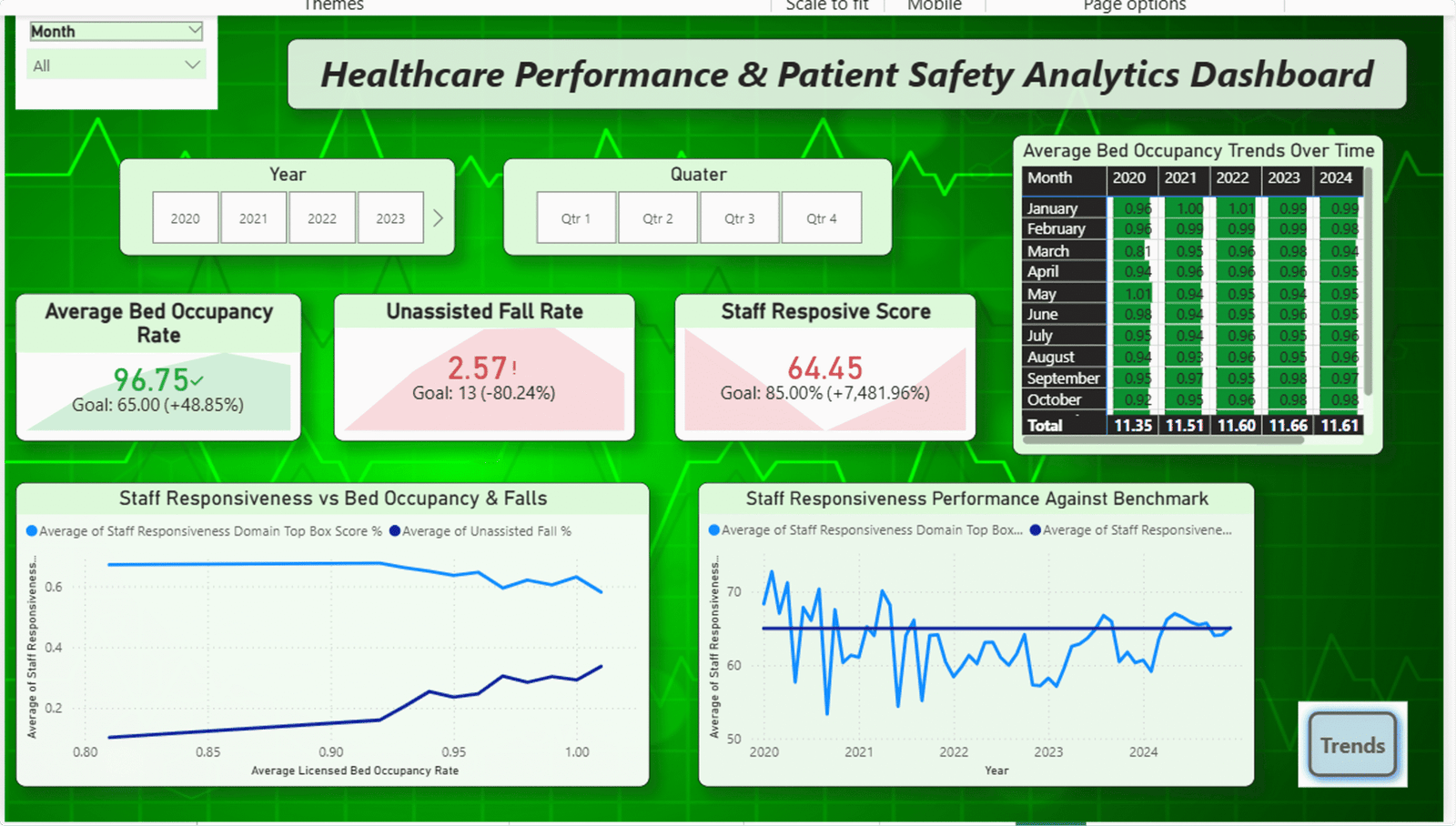
A KPI-Driven Study of Lowell General Hospital
Business Context :
Lowell General Hospital places patient well-being at the core of its care delivery model. While maintaining a strong reputation for quality and safety, hospital leadership recognizes that patient dissatisfaction can arise from multiple operational and clinical factors.
To ensure patients continue to receive safe, responsive, and high-quality care, management initiated a data-driven analysis of key healthcare performance and patient safety metrics to better understand their impact on patient experience.
Problem Statement :
Despite a strong commitment to patient-centric care, variations in hospital operations and safety outcomes may influence patient satisfaction.
A structured analysis of critical KPIs is required to:
Identify performance trends
Evaluate relationships between operational efficiency, staff responsiveness, and patient safety
Detect potential areas of risk impacting patient experience
Objectives :
Assess the impact of key healthcare KPIs on patient experience and safety
Analyze correlations between operational and safety metrics
Benchmark hospital performance against defined standards
Provide data-driven recommendations to enhance patient satisfaction and care quality
Key Metrics Analyzed:
Average Licensed Bed Occupancy Rate
Staff Responsiveness – Top Box Score
Unassisted Fall Rate per 1,000 Patient Days
Key Variables Analyzed :
Month
Average Licensed Bed Occupancy Rate
Unassisted Fall Rate per 1,000 Patient Days
Staff Responsiveness – Domain Top Box Score
Dataset preview :
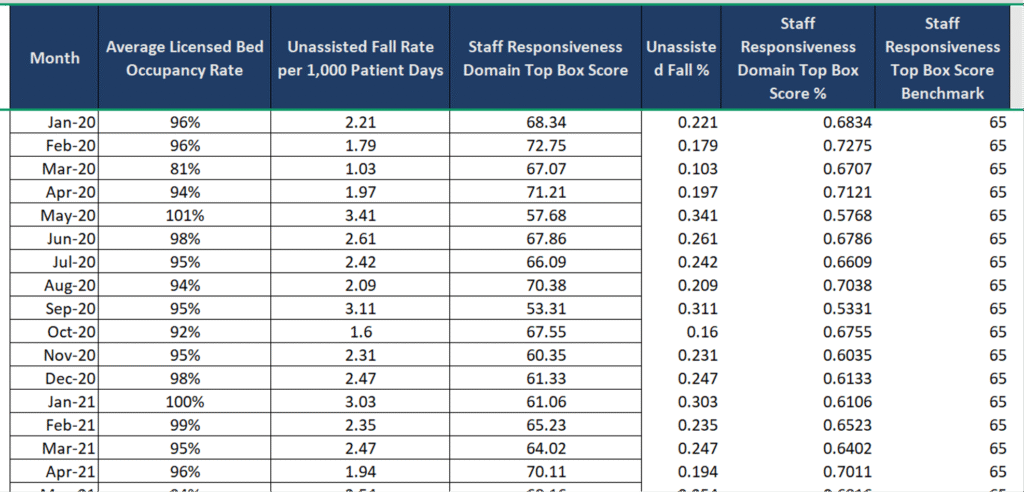
Understanding KPIs :
Average Licensed Bed Occupancy Rate
Purpose:
Measures hospital capacity utilization and operational efficiency
Captured internally and reported as a percentage
Indicates how effectively licensed beds are being utilized over time
High occupancy may impact staff workload and patient experience
Calculation:

Staff Responsiveness –Top Box Score
Purpose:
Measures patient perception of staff responsiveness and quality of care
Derived from the Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) survey
Collected post-discharge from patients
Based on responses to two key questions:
Timeliness of help after pressing the call button
Timeliness of assistance with bathroom use or bedpan
Top Box Definition:
Percentage of patients who responded “Always” to both questions
Calculation:

Unassisted Patient Falls per 1,000 Patient Days
Purpose:
Measures patient safety and fall-prevention effectiveness
Sourced from the National Database of Nursing Quality Indicators (NDNQI)
A fall is defined as an unplanned descent to the floor, with or without injury
Unassisted falls occur when no staff member is present to help the patient
Calculation:

Metrics
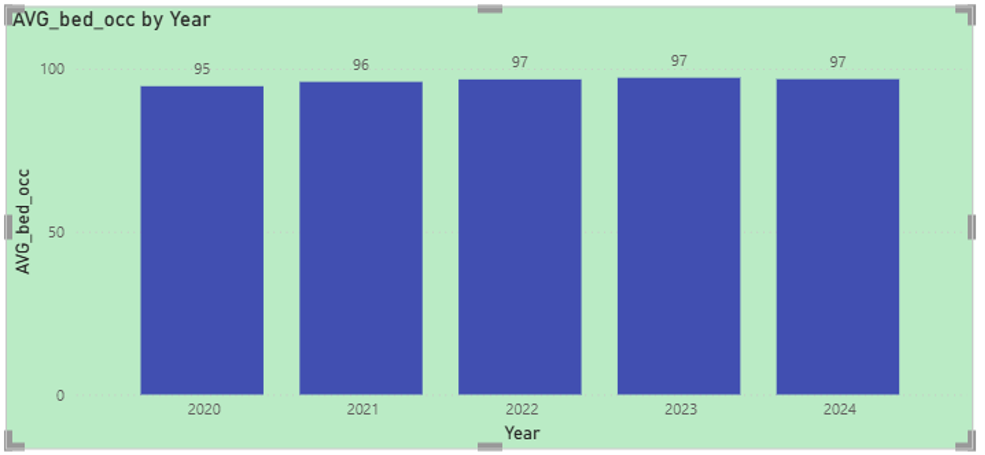
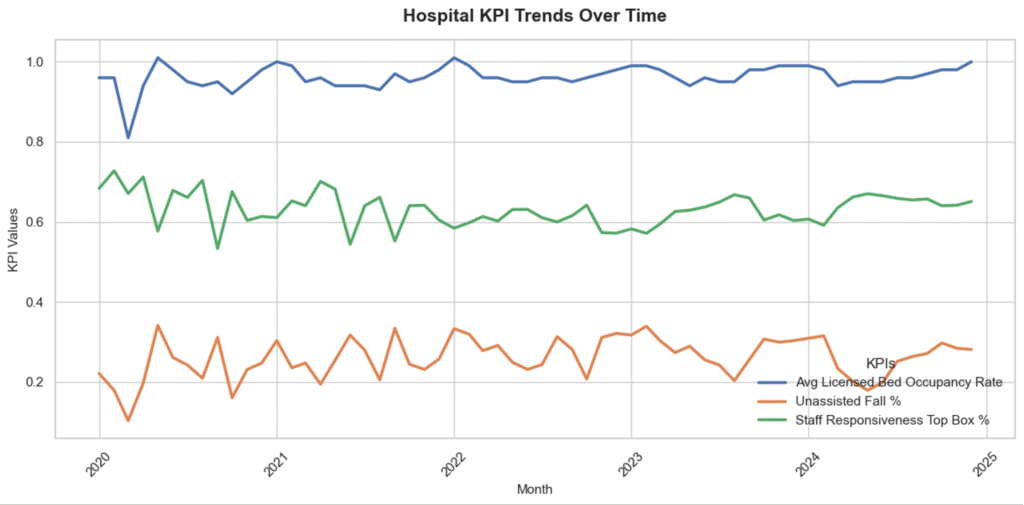
- Average Licensed Bed Occupancy Rate :
- Bed occupancy levels remained consistently high throughout the period
- Increased slightly from 95% in 2020 to approximately 97% from 2022 through 2024
- This stability reflects strong and sustained utilization of licensed bed capacity, indicating high operational demand
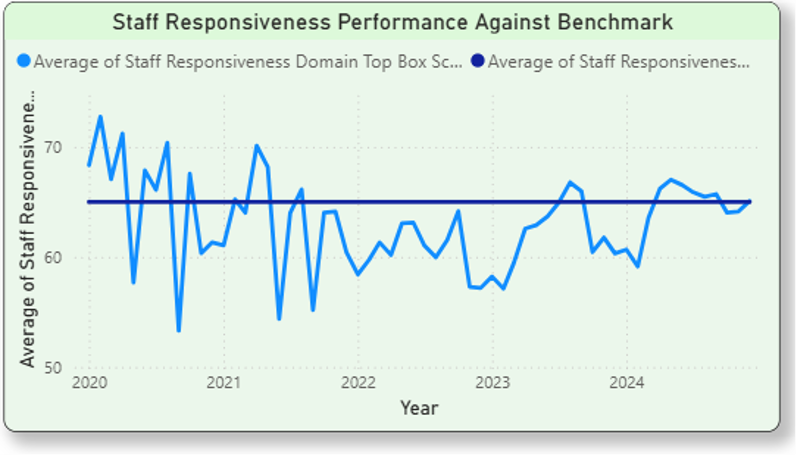
- Staff Responsiveness – Top Box Score (%) :
- Staff responsiveness scores declined from 65% in 2020 to 61% in 2022
- A gradual recovery was observed, reaching 64% by 2024
- While recent improvements suggest corrective efforts are having some impact, overall responsiveness remains an area requiring continued focus
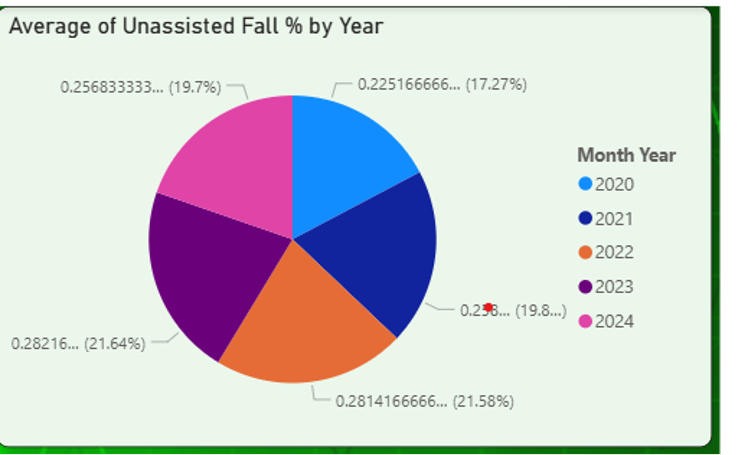
- Unassisted Patient Falls (%) :
- The percentage of unassisted falls
- increased from 23% in 2020 to 28% in
- 2022 and 2023
- A slight reduction to 26% was observed
- in 2024
- This pattern indicates ongoing patient
- safety risks, highlighting the need
- for strengthened fall-prevention
- strategies.
Relationship Between KPIs :
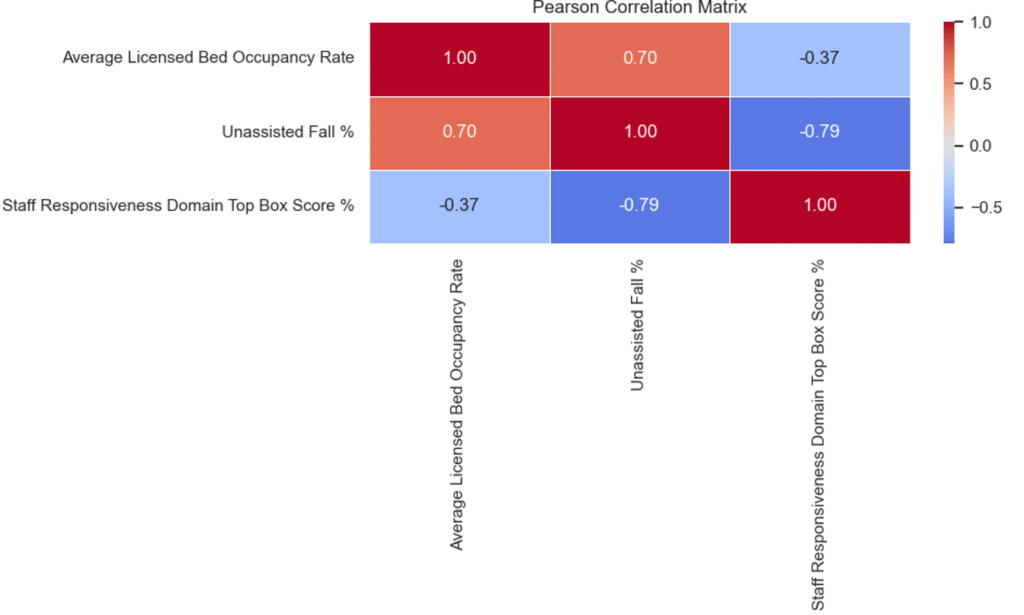
- Correlation Analysis Summary :
- Bed Occupancy Rate vs. Unassisted Fall Rate (per 1,000 Patient Days)
- Correlation: +0.70 (Strong Positive Relationship)
- Higher bed occupancy levels are associated with an increase in unassisted patient falls, suggesting potential strain on staff capacity during periods of high utilization.
- Bed Occupancy Rate vs. Staff Responsiveness – Top Box Score
- Correlation: −0.37 (Moderate Negative Relationship)
- As bed occupancy increases, staff responsiveness scores tend to decline, indicating possible operational pressure impacting timely patient assistance.
- Unassisted Fall Rate (per 1,000 Patient Days) vs. Staff Responsiveness – Top Box Score
- Correlation: −0.79 (Strong Negative Relationship)
- Lower staff responsiveness is strongly associated with higher unassisted fall rates, highlighting staff responsiveness as a critical driver of patient safety outcomes.
- 💡 Key Insight
- High bed occupancy may indirectly affect patient safety by reducing staff responsiveness, leading to increased unassisted falls.
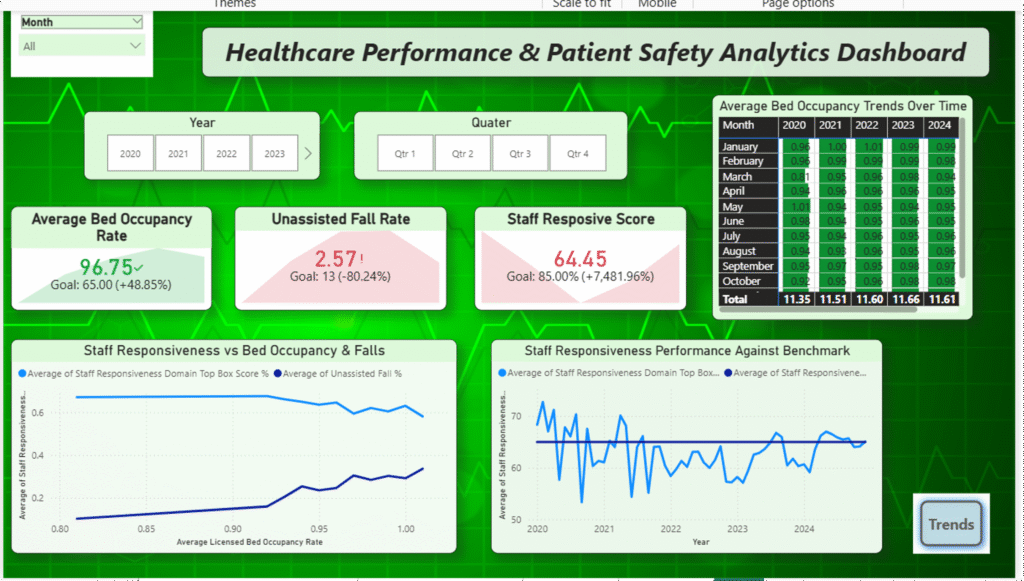
Visualization using PowerBi
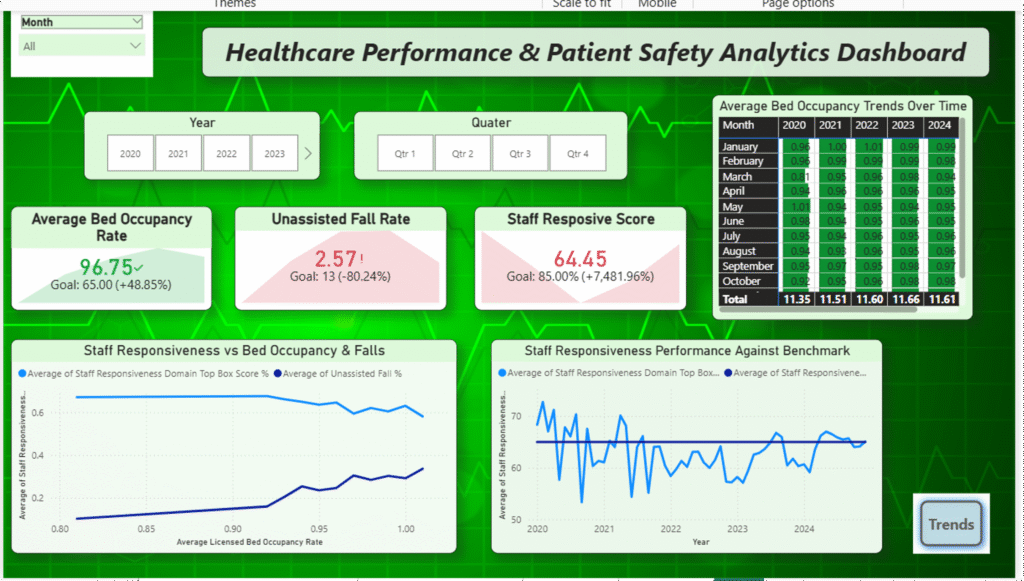
Summary of Insights & Findings :
- Analysis of key KPIs at Lowell General Hospital highlights strong interdependencies between bed occupancy, staff responsiveness, and patient safety. A strong positive correlation (r = +0.70) indicates that higher bed occupancy is associated with increased unassisted fall rates, suggesting operational strain during high-demand periods.
- Bed occupancy also shows a moderate negative relationship with staff responsiveness (r = −0.37), implying that rising patient volumes may impact staff availability.
- Staff responsiveness demonstrates a strong negative correlation with unassisted falls (r = −0.79), confirming its critical role in patient safety outcomes.
- Findings show consistently high bed occupancy, responsiveness challenges during peak periods, and increased fall rates with higher occupancy.
Key Recommendations
Optimized Staff-to-Patient Ratios –
Maintaining an appropriate staff-to-patient ratio is essential to prevent staff overload, ensure timely patient assistance, and reduce the likelihood of unassisted falls—particularly during periods of high bed occupancy.
Targeted Staff Training & Responsiveness Enhancement –
Focused training programs aimed at improving staff alertness, responsiveness, and proactive patient monitoring—especially during peak occupancy periods—can significantly enhance patient safety and lower fall risks.
Adaptive Operational Planning –
Staffing levels should be reviewed and adjusted dynamically based on real-time bed occupancy trends to maintain consistent care quality, reduce operational strain, and support patient safety across all demand levels.
Conclusion
Sustaining optimal bed occupancy levels, supported by responsive and well-trained staff, is critical to improving patient safety and overall hospital performance. Long-term success relies on continuous optimization of staffing strategies, ongoing training initiatives, and proactive operational planning aligned with patient demand.